The emerging realm of telemedicine software development offers a unique solution for healthcare providers and patients to interact remotely, enhancing healthcare delivery access, efficiency, and convenience. But we only got to taste its immense benefits not so long ago. Did you know that during COVID-19, 82% of Americans tried telehealth for the first time? And only after three years, in 2022, almost 40% of patients already received care via telemedicine apps.

After the global pandemic, telehealth has quickly transitioned from an innovation to a basic healthcare service. This recent shift towards virtual care has spurred the need for a robust, reliable, and feature-rich telemedicine application. So let us explore the world of telemedicine app development, its importance, development process, cost implications, requirements, etc.
Are you ready to revolutionize your care delivery? Contact SPsoft to learn how our telemedicine software development services can help you launch a scalable, secure, and user-centric platform that transforms the patient journey!
Table of Contents
“Our team has always strived to be pioneers in the realm of health tech, and our approach to telemedicine software development is no exception. SPSoft’s commitment to bringing your custom telemedicine software solutions to life will reshape the industry’s landscape and make a significant, tangible impact in the lives of your patients.”
Romaniya Mykyta
Head of Product Management, SPSoft
“Our dedication to revolutionizing healthcare with innovative telemedicine software development is undeniable — you’ll notice it from the get-go. Working with SPSoft will propel your project into the next level of care provision and allow you to touch patients’ lives in new and meaningful ways.”
Mike Lazor
CEO, SPSoft
Overview of Today’s Telemedicine Market
Telemedicine is a growing sector within the healthcare industry, driven by technological advancements and increasing demand for convenient, accessible healthcare solutions. The COVID-19 pandemic significantly accelerated the growth of the industry, as people turned to virtual consultations to minimize the risk of virus transmission. Many healthcare companies rapidly adopted telemedicine technology to continue providing services during lockdowns.

As a result, the telemedicine market size stands at $70B as of 2023, compared to $46.4B pre-Covid. Powered by technologies like 5G and artificial intelligence, it is expected to reach more than $200B by 2030.
Three Major Types of Telemedicine Solutions
Off-the-shelf and custom telemedicine software solutions are designed to address a broad spectrum of health concerns and come in three main varieties — real-time telemedicine, store-and-forward telemedicine, and remote patient monitoring (RPM).
Real-Time Telemedicine
Real-time telemedicine services are interactive and leverage secure video conferencing or a telehealth app that is a virtual substitute for traditional consultations. Subcategories include:
- telepsychiatry
- telenursing
- telepharmacy
- telerehabilitation
- teleneuropsychology
Healthcare providers, including primary care physicians and psychiatrists, use telemedicine software development services most often as they facilitate immediate care delivery, particularly in emergencies, and for follow-up visits or monitoring medication regimes.
Store-and-Forward Telemedicine
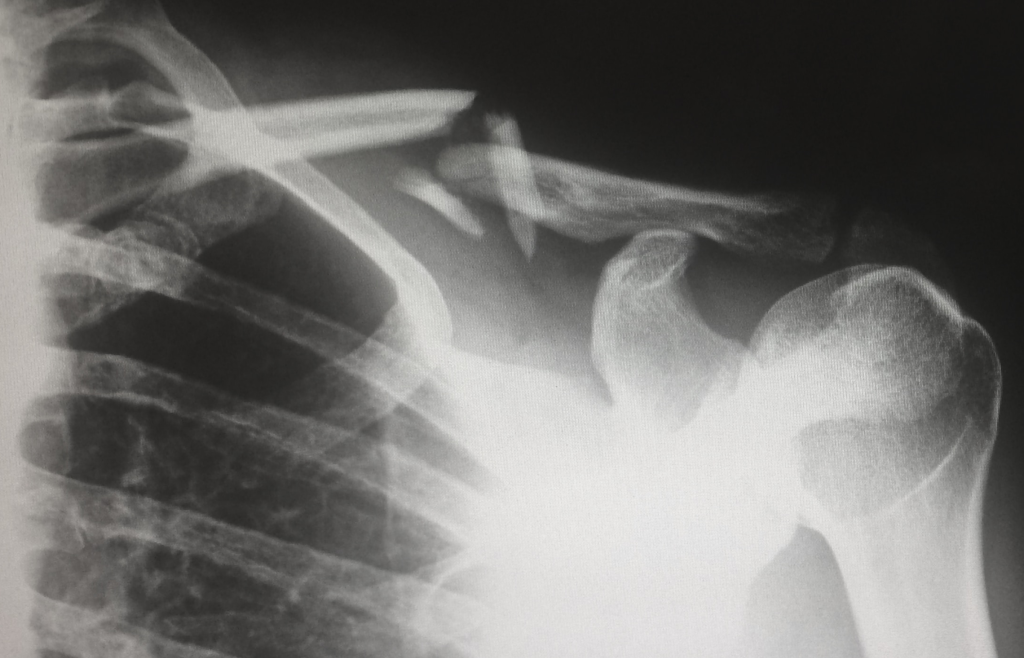
Also known as asynchronous telemedicine, this telemedicine solution relies on the electronic transmission of health data between patients and physicians. It can include sharing laboratory reports, images (MRI scans and X-rays), and audio and video studies. This principle underpins implementing internal electronic health record (EHR) systems within a healthcare organization, enhancing its operational efficiency.
Remote Patient Monitoring
Telemonitoring encompasses the use of IoMT wearable devices like heart monitors, skin patches, or smartwatches that gather critical vitals. This data is then transmitted to applications on devices and eventually sent to a cloud computing server for analysis.
Remote patient monitoring is generally adopted for patients managing chronic conditions such as diabetes, asthma, or cardiovascular disease. It also enables medical specialists to continue monitoring their patients’ health even after discharge, facilitating a return to their regular life while ensuring patient safety.
Trends in Telemedicine Technologies
Telemedicine development is increasingly becoming an integral part of the healthcare industry and is being rapidly transformed by technological advancements like the following.
Artificial Intelligence (AI) and Machine Learning (ML)
AI and ML are used to analyze patient data, predict health trends, and help doctors diagnose conditions. They are also used in managing appointments and maintaining electronic health records. Also, AI predictive analytics can warn early about potential health crises or outbreaks.
Internet of Medical Things (IoMT)
The IoMT is a connected network that generates, collects, analyzes, and transmits health data. The network can include medical devices and wearable technology such as smartwatches, fitness trackers, and home health monitors that send data directly to healthcare providers. The latter can then make informed decisions about their patients’ well-being.
5G Technology
The introduction of 5G allows for higher data transfer speeds and lower latency, enabling mobile telemedicine through real-time remote patient monitoring and high-quality video consultations. 5G may also enable remote surgery, with doctors operating on patients from miles away with the help of robotic systems and real-time data transmission.
Blockchain Technology
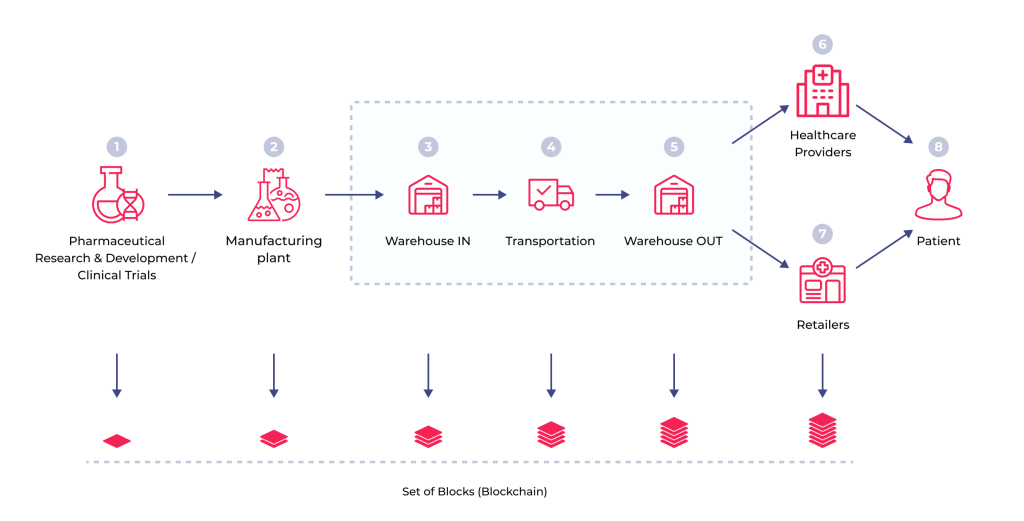
Blockchain’s ability to provide secure, transparent, and tamper-proof health records is increasingly recognized as a vital telemedicine feature. It can help maintain patient privacy, ensure data integrity, and manage patient consent. Furthermore, blockchain enhances supply chain transparency, ensuring patients treated remotely receive authentic medication.
Augmented Reality (AR) and Virtual Reality (VR)
AR and VR technologies can be used for medical training, patient education, and therapeutic purposes. Such techs enhance patient outcomes, helping providers better explain diagnoses and treatment plans. Moreover, AR and VR are being explored for therapeutic processes, such as pain management and psychological therapy.
Cloud Computing
Cloud technology in telemedicine allows for the efficient storage and sharing of large amounts of patient data. It can also facilitate integration and interoperability between different healthcare systems, streamlining workflows and promoting collaboration among healthcare professionals.
Telemedicine Software Development — Who Needs It?
Telemedicine software development is helpful for various healthcare professionals, institutions, and patients. Here are some of its potential users and applications:
- Healthcare providers can extend their services beyond their physical offices, providing remote healthcare to patients who may not be able to travel for in-person visits.
- Hospitals and clinics can provide complex patient care by monitoring patients’ health remotely, conducting follow-ups, providing urgent care services, and reducing wait times.
- Pharmacies can use telemedicine software and devices to consult with patients, recommend over-the-counter medications, and provide medication management services through a robust web app.
- Health insurance companies can incorporate management software into their services to streamline claim processing, provide health advice, and offer preventative care services to their policyholders.
- Patients, especially those living in remote areas, with mobility issues or busy schedules, can use a telehealth solution to consult with healthcare providers, manage their health records, and monitor overall health conditions.
Telemedicine development requires understanding the needs of such diverse users, including their workflow, communication channels, and data security requirements. So, working with an experienced telemedicine software development company is vital to guarantee your telehealth platform is functional and secure.
How Telemedicine Solutions Work
When a healthcare provider offers telehealth options, an individual requires a mobile app or computer to connect.
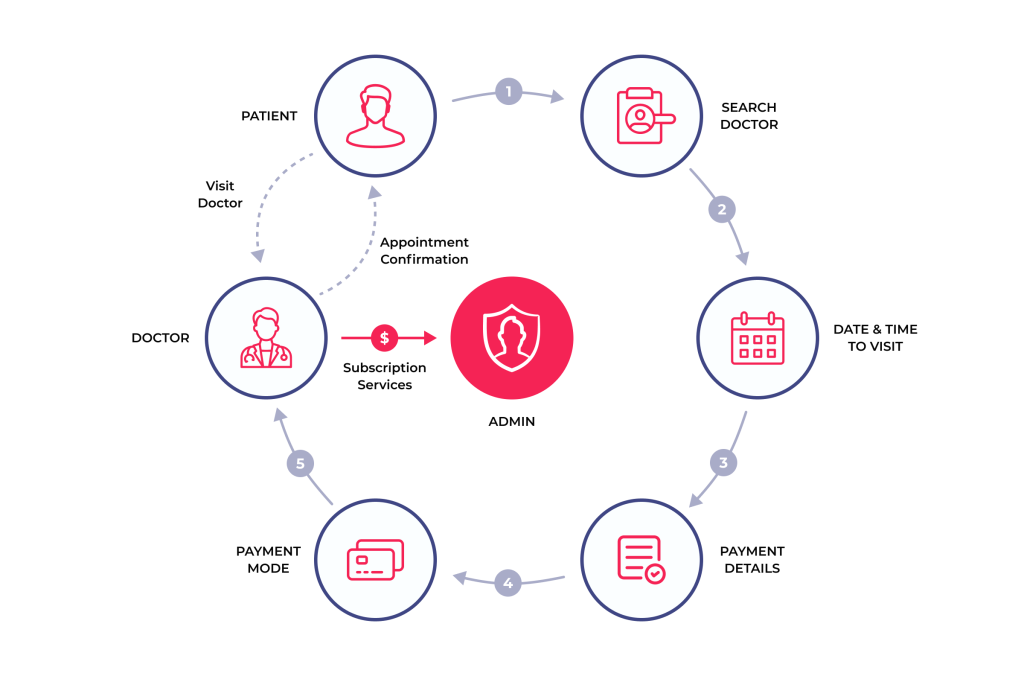
The patient interface allows patients to view their medical history, interact with healthcare professionals via messages, request refills of prescriptions, and schedule appointments online. Even if the patient has to visit the doctor physically, the prior arrangements can be done from the comfort of their home.
The doctor’s interface allows healthcare professionals to access health records, manage patient interactions, set up appointment schedules, and provide consultations. This interface offers a comprehensive view of the patient’s medical history, test results, medication details, and past consultation notes, facilitating a holistic understanding of the patient’s health status.
Doctors can also track treatment progress, make necessary adjustments to the treatment plan as needed, and send prescriptions digitally to the pharmacy of the patient’s choice. That helps minimize the need for physical prescription handovers, all within a single telemedicine system.
Building a Telemedicine Platform: The Main Features
A successful telemedicine platform usually has many capabilities to facilitate remote healthcare services. Here are some of the key features:
- video conferencing
- scheduling and appointment management
- EHR integration
- prescription management
- secure messaging
- payment processing
- mobile access via a telehealth app
The exact telemedicine software features can vary based on whether you are building a web app or a native mobile app.
The Undeniable Benefits of the Telemedicine Technology
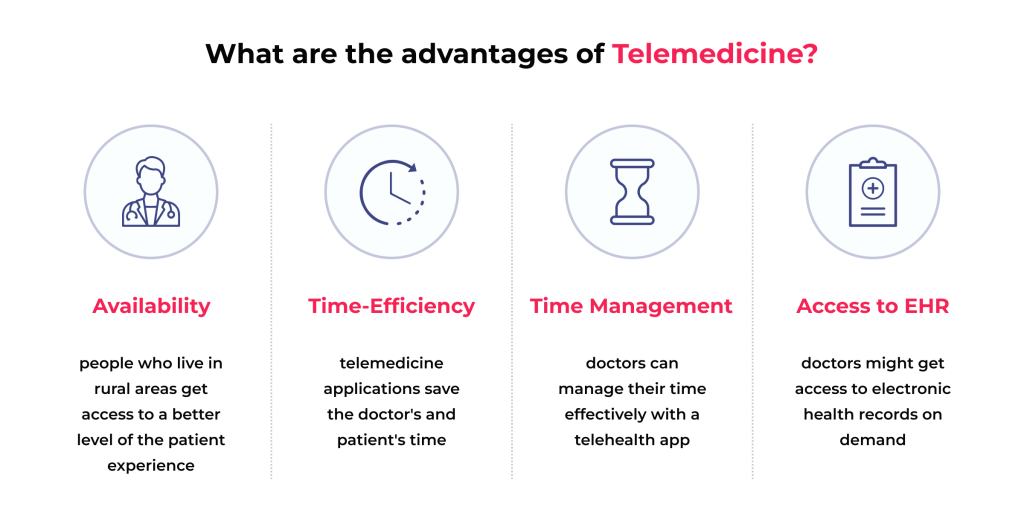
Telemedicine software development offers some benefits to patients and healthcare providers:
- Availability — more accessible medical services for people living in rural areas or struggling to reach the doctor’s office physically.
- Time efficiency — both patients and doctors save time on the commute without sacrificing the quality of care.
- Improved time management — practice management software allows for more flexibility for patients and better workday planning for physicians.
- Faster access to patient data — doctors can use EHRs to get a full overview of a patient’s vitals within their healthcare system.
Overall, telemedicine offers excellent advantages and brings healthcare services closer to patients and doctors, regardless of location or availability.
Examples of the Most Successful Telemedicine Solutions
With various off-the-shelf and custom telemedicine software solutions available, some tend to stand the test of time. Here are three best telemedicine platforms recognized as leading ones:
1. Teladoc
Teladoc Health, typically referred to as Teladoc, is a multinational telemedicine and virtual healthcare company. It allows patients 24/7 access to healthcare services via mobile devices, the Internet, video, or phone. The company’s broad services encompass general medical consultations, dermatology, mental health, and specialized expert medical assistance.
2. Amwell
Amwell (American Well) is another key player in the telehealth industry. They connect users with doctors, therapists, and medical specialists through video conferencing. The services provided by Amwell range from urgent care to chronic disease management to preventative health care. In addition to serving individual patients, they also offer services for health systems, insurers, and employers. They bring a suite of tech and software to enable other healthcare organizations to build their own telehealth system.
3. Doctor on Demand
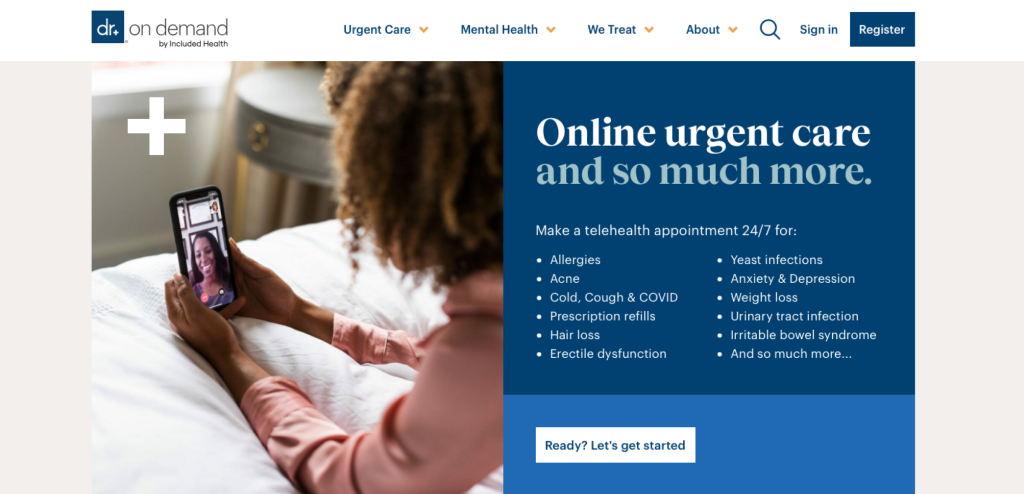
Doctor on Demand, arguably one of the most renowned telehealth apps, is known for its rapid service, connecting patients with doctors in just three minutes for a video consultation with a doctor. After the consultation, the physician provides a diagnosis and recommends appropriate treatment securely stored in an EHR system or cloud storage.
Telemedicine Software Requirements
Developing a telemedicine platform brings numerous advantages to healthcare services but also comes with its own requirements. Here are some of them.
Technical Requirements
Telemedicine software and devices require a reliable, high-speed internet connection for video consultations and data transmission, which is not often available in some areas or for some patients. Also, patients and providers need to have hardware that is capable of running it.
User Experience
While telemedicine improves access to healthcare services, it may also exacerbate disparities if some populations (elderly, rural, low-income, or less tech-savvy individuals) cannot use them. Thus, a well-thought UX design is crucial to ensure the software is intuitive and user-friendly.
Data Security and Privacy
Telemedicine platforms deal with sensitive personal and medical data, making them potential cyberattack targets. Robust security measures must be in place to protect it. Compliance with healthcare regulations like HIPAA and GDPR is mandatory for HIPAA-compliant telemedicine.
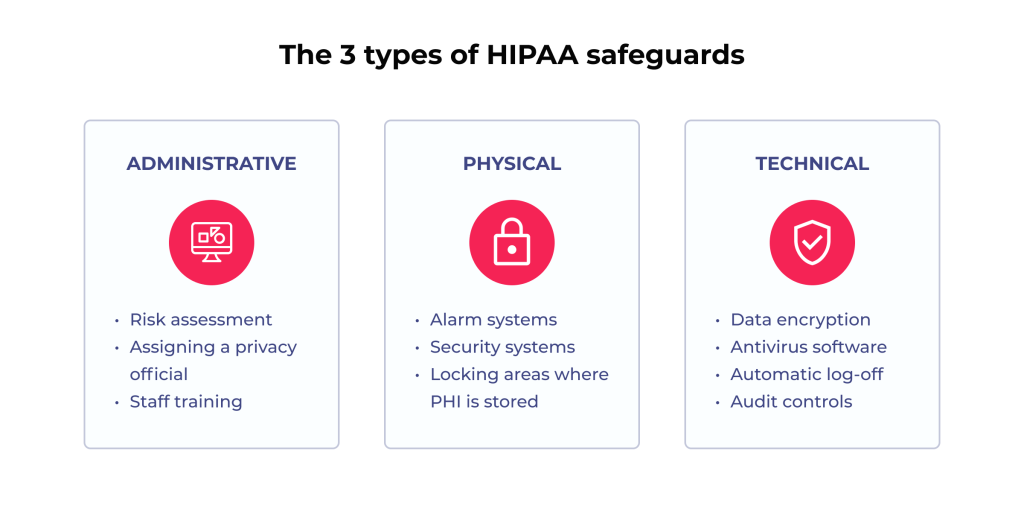
Of course, addressing these requirements involves careful planning and ongoing technical support. But the outcome is a secure, well-functioning telehealth platform.
The Process Behind Telemedicine Software Development
The telemedicine software development process is complex. It requires technical expertise and a deep understanding of healthcare operations and rules. Here is the process, step by step:
- Requirement gathering and analysis. The first step involves understanding the healthcare organization’s needs, their workflows, the types of services required, data management demands, and the tech and regulatory environment in which they operate.
- Design. Once the requirements are clear, the next step is designing the user interface for your telehealth application, data structures, functional modules (video consultations, appointment scheduling, prescription management), and the security measures.
- Development & integration. This step involves the development team translating the design into a functional application. This stage also covers integrating the software with other healthcare systems like EHRs, billing systems, pharmacies, and medical devices.
- Testing & deployment. Testing involves running the app under a variety of conditions and use cases. Once the software has been tested and refined, it can be installed on the users’ devices or go live for online access.
- Training and maintenance. Training implies educating users during the development process on how to deal with the software properly. Ongoing maintenance is essential to ensure the software is updated regularly and continues operating smoothly and securely.
Final Word
High-quality, custom telemedicine software and devices reshape healthcare delivery, making it more accessible, convenient, and patient-centric than ever before. So, investing in telemedicine software development today can yield outstanding pros in improved patient care and enhanced healthcare outcomes in the long run. Whether starting from scratch or optimizing an existing system, we hope this guide provides the insights you need to embark on your relevant journey.
Navigating the complexities of HIPAA-compliant telemedicine development requires a partner with deep domain expertise. Message SPsoft’s experts to receive a detailed cost estimate and a strategic roadmap for building your custom telemedicine app!
FAQ
What hardware and software are used for telemedicine?
Telemedicine usually involves using hardware like personal devices (smartphones, tablets) and medical devices like blood pressure monitors. As for medical software, the most common solutions include a telemedicine platform for video calls, an electronic health record (EHR) for data storage, and custom software for secure messaging. Software developers often integrate these components into a unified telehealth system that allows healthcare providers to enable healthcare delivery remotely while maintaining high standards of patient care.
What is telemedicine software?
Telemedicine software is a digital software solution that facilitates remote clinical medical services, enabling healthcare professionals and patients to interact without being in the same location. This telemedicine solution leverages telehealth tech to facilitate virtual consultations through secure video, voice, or messaging. By developing a telemedicine system, organizations can create telemedicine workflows that bridge geographical gaps and enable healthcare providers to reach more patients through a web app or mobile app.
How do I build a telemedicine platform?
To build a telemedicine platform, you must first define your intended use and target audience. The telemedicine software development process begins with requirement analysis, followed by UI/UX design and application development. You must hire app developers who understand healthcare regulations and can develop custom features like EHR integration. A reliable software development partner will guide you through the development process, ensuring that you build a telemedicine app that is secure and user-friendly for all healthcare professionals.
What is the average telemedicine app development cost?
The telemedicine app development cost varies based on the telemedicine software features and the complexity of the app. On average, a standard telemedicine platform costs between $90,000 and $200,000. Factors influencing the cost of a telemedicine app include the hourly rates of development companies, the type of mobile app development (native vs. cross-platform), and the number of integrations with third-party systems. Choosing an experienced app development company helps in optimizing the development cost while ensuring its successful launch.
What are the main features of telemedicine software?
The features of telemedicine typically include high-definition video conferencing, secure patient data messaging, and appointment scheduling. Advanced telemedicine software solutions also feature electronic health record integration, digital prescription management, and payment processing. For healthcare providers, a practice management software module is often included to track clinician roles. A scalable telemedicine platform ensures such features work seamlessly across both web app and mobile app environments to improve patient outcomes.
How does telemedicine app development ensure HIPAA compliance?
Telemedicine app development ensures compliance by adopting the three HIPAA safeguards: administrative, physical, and technical. Software developers use data encryption for health data in transit and at rest, alongside multi-factor authentication for login. Besides, a HIPAA-compliant telemedicine software solution includes automated audit logging to track access to health records. Working with a telehealth software development company with a proven development process is the best way to ensure your telemedicine application meets all legal requirements.
Why should I choose a custom telemedicine software development company?
Choosing a custom telemedicine software development firm like SPsoft allows you to build a custom telemedicine app tailored to your specific clinical workflow. Unlike generic solutions, custom telemedicine software solutions can be integrated with your existing healthcare system and branded to your clinic. An experienced telemedicine app development company can develop telemedicine tools that are scalable and include remote patient monitoring modules. That ensures the best telemedicine experience for both patients and healthcare providers.
What are the steps in the telemedicine software development process?
The telemedicine software development process follows a structured lifecycle: Requirement Analysis, Design, Application Development, Integration, Testing, and Deployment. Throughout the development process, the development team works closely with healthcare providers to ensure the telemedicine system meets clinical needs. After the initial launch, maintenance and updates are required to keep the telehealth app compatible with new mobile device operating systems. A reliable telehealth software development partner like SPsoft ensures transparency throughout the development process for a high-quality telemedicine platform.



